Burton Latimer dementia patient waited two years for diagnosis


A Burton Latimer man diagnosed with Alzheimer’s disease after nearly two years of uncertainty and being told his symptoms were depression and anxiety has said his diagnosis was a ‘breath of fresh air’.
When Peter Middleton, from Burton Latimer, was diagnosed with dementia in 2019 at the age of 64, it finally explained why he was behaving out of character – failing to keep deadlines and missing meetings.
Advertisement
Hide AdAdvertisement
Hide AdNew Alzheimer’s Society research launching Dementia Action Week from May 16 to 22 reveals confusing symptoms with old age is one of the main reasons for delay.

A survey of more than 1,000 people with diagnosed dementia, carers and people without a diagnosis, found more than a third in the in East Midlands lived with the condition for more than two years after first noticing their symptoms, before getting a diagnosis.
Peter, a former Police Community Support Officer in Northampton, said: “I finally had an answer to why I had been behaving so out of character.
“I would miss deadlines and turn up to work meetings at the wrong time or place. This was really out of character and I couldn’t work out why I was making mistakes like this.
Advertisement
Hide AdAdvertisement
Hide Ad“I sought help from my GP and within a five-minute conversation I was given a diagnosis of depression and anxiety – I knew deep down it wasn’t that, as did my wife Pam.
“During this time, we had a new doctor start within the police force. After listening to me she was the first person to mention the possibility of dementia. I eventually had a brain scan which did show shrinkage and my Alzheimer’s diagnosis was confirmed.”
The figures also showed a further 26 per cent of people in the East Midland region waited between one and two years for their diagnosis.
One of the main reasons for delay was that they assumed the symptoms were just part of getting old, leading to a delay in accessing treatment, care and support.
Advertisement
Hide AdAdvertisement
Hide AdDementia describes a group of symptoms that include problems with memory, thinking or language, and changes in mood, emotions, perception and behaviour. Dementia is caused by diseases of the brain and is not a natural part of ageing.
In a bid to tackle the problem, Alzheimer’s Society has launched a new campaign – ‘It’s not called getting old, it’s called getting ill’ – to encourage people worried about their own or their loved ones’ memory to seek support in getting a diagnosis.
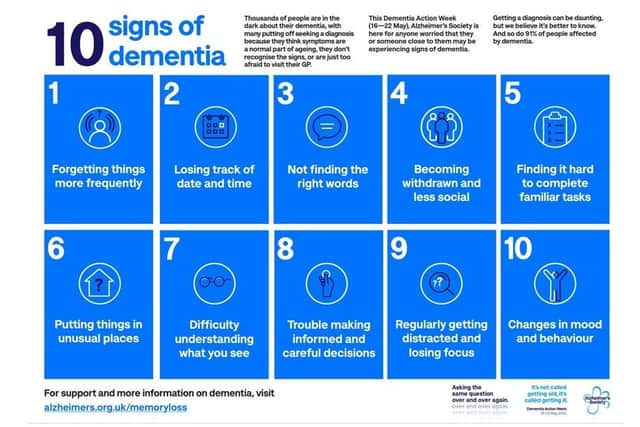
The charity has worked closely with leading clinicians to make the diagnosis process easier, developing a new ‘symptoms checklist’, available on their new online hub, highlighting changes that might be due to dementia.
Tina Kierman, Alzheimer’s Society’s area manager in Northamptonshire, said: “Asking the same question over and over again is not called getting old, it’s called getting ill. If you’re worried for yourself or someone you love, take the first step this Dementia Action Week – come to Alzheimer’s Society for support.
Advertisement
Hide AdAdvertisement
Hide Ad“The stark findings of our survey show just how dangerous it can be to battle dementia symptoms alone and put off getting help.
“Yes, getting a diagnosis can be daunting, but it is worth it. More than nine in 10 people with dementia told us they benefited from getting a diagnosis – it gave them crucial access to treatment, care and support, and precious time to plan for the future.
“With the pandemic causing diagnosis rates to plunge, it’s more important than ever to seek help. You don’t have to face dementia alone, we’re here to support everyone affected.”
There are 900,000 people living with dementia in the UK, including more than 69,500 across East Midlands.
Advertisement
Hide AdAdvertisement
Hide AdAlzheimer’s Society’s survey also revealed more than a quarter of those who were diagnosed after two years in East Midlands, only sought a diagnosis because symptoms were no longer manageable, with 13 per cent saying they reached crisis point, finding it difficult to cope. A third in the region sought a diagnosis after two years because they needed more help to continue daily activities.
More than 200,000 people will develop dementia this year, the equivalent of one person every three minutes. But with diagnosis rates at a five-year low, tens of thousands of people are now living with undiagnosed dementia without access to the vital care and support that a diagnosis can bring.
Dr Jill Rasmussen, the clinical representative for dementia at the Royal College of General Practitioners, said: “It’s vital for patients, their families and GPs that conversations with the potential for a diagnosis of dementia are timely and effective.
“The new checklist developed with Alzheimer’s Society is a simple, free tool to help patients and their families clearly communicate their symptoms and concerns during an often time-pressured appointment.
Advertisement
Hide AdAdvertisement
Hide Ad“This resource could make a real difference in identifying those people who require referral for a more detailed evaluation and diagnosis of their problems. We’re asking anyone who is worried about possible dementia symptoms to use the checklist and share it with their primary care team.”
This Dementia Action Week, Alzheimer’s Society is urging anyone worried about themselves or someone they love to take the first step and contact the charity for support.
Visit alzheimers.org.uk/memoryloss or call 0333 150 3456. For callers who do not have English as their language of choice, Alzheimer’s Society can arrange a simultaneous language translation service.