People who experience ‘mild’ coronavirus symptoms may have serious neurological complications - here’s what doctors are saying
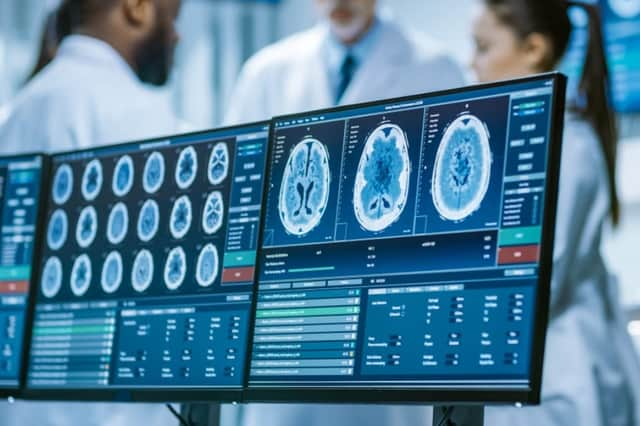

As researchers and experts continue to get to grips with coronavirus, scientists have warned that the signs of potentially life changing brain disorders in sufferers are being missed by many doctors.
Findings published by neurologists on 8 July reveal the details of nearly 50 Covid-19 patients who developed potentially fatal complications, from brain inflammation to nerve damage and stroke. In many cases, they were otherwise only "mildly" affected by coronavirus.
Advertisement
Hide AdAdvertisement
Hide AdAccording to the report, a dozen patients had inflammation of the central nervous system, 10 had brain disease with delirium or psychosis, eight had strokes, and a further eight had peripheral nerve problems.
A 59 year old woman died of Covid-19 triggered neurological problems. It is thought such fatalities could affect up to five per cent of those affected by the disease.
What is ‘Adem’?
Published in the journal, Brain, the research revealed a rise in cases of Adem (acute disseminated encephalomyelitis) - a life-threatening condition that became more commonplace as the coronavirus crisis spread through the UK.
Cases rose from one a month before the pandemic to two or three per week in April and May at UCL’s Institute of Neurology.
Advertisement
Hide AdAdvertisement
Hide AdAdem is a rare autoimmune disease, often triggered by a viral infection. Its main symptoms include a sudden, widespread attack of inflammation in the brain and spinal cord as it attacks and damages the nerves of the central nervous system.
Michael Zandi, a senior author on the study and a consultant at the institute and University College London Hospitals NHS foundation trust, said, “Biologically, Adem has some similarities with multiple sclerosis, but it is more severe and usually happens as a one-off.
"Some patients are left with long-term disability, others can make a good recovery.

“We’re seeing things in the way Covid-19 affects the brain that we haven’t seen before with other viruses.
Advertisement
Hide AdAdvertisement
Hide Ad“What we’ve seen with some of these Adem patients, and in other patients, is you can have severe neurology, you can be quite sick, but actually have trivial lung disease."
What does it mean for Covid-19 patients?
The findings come at a time when the long-term effects of Covid-19 are only beginning to be understood, with many patients left breathless and fatigued long after they have cleared the virus. Others have reported numbness, weakness and memory problems.
One patient in the paper began to hallucinate the day after her initial discharge from hospital, reporting that she saw monkeys and lions at home.
“We want clinicians around the world to be alert to these complications of coronavirus,” said Zandi, urging doctors whose patients exhibit cognitive symptoms to discuss their case with neurologists.
“The brain does appear to be involved in this illness.”
Advertisement
Hide AdAdvertisement
Hide AdThe 55 year old woman - with no history of psychiatric illness - was readmitted to hospital, and her symptoms improved after a course of antipsychotic medication.
What does it mean for the future?
Despite the new research, there is still much to be learned on Covid-19.
The full range of disorders caused by the disease could be hard to define, as many patients are too unwell to examine properly.
One fear is that neurological issues caused by Covid-19 may lay dormant, before re-emerging in a few years' time.
Advertisement
Hide AdAdvertisement
Hide Ad“It’s a concern if some hidden epidemic could occur after Covid where you’re going to see delayed effects on the brain, because there could be subtle effects on the brain and slowly things happen over the coming years, but it’s far too early for us to judge now,” Zandi said.
It is believed a similar scenario emerged following the 1918 flu pandemic, which is thought to have left up to a million people with a brain disease.
“We hope, obviously, that that’s not going to happen, but when you’ve got such a big pandemic affecting such a vast proportion of the population it’s something we need to be alert to.”